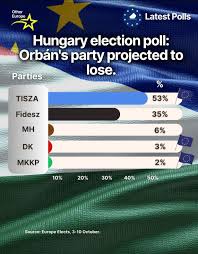
The cats have decided that the living room carpet under the piano is some sort of third litter box. I have moved from placing pads to bopping them on the nose when I catch them. I suppose the next step is to pull a Susan Collins and tell them of my great concern in a sternly worded letter. As anti-Republican sentiment continues to rise over the execrable behavior at the top of the party, it appears that no amount of attempts at moderation through gravely troubled rhetoric, while continuing to vote the party line, is likely to save her her seat. There’s a lot of worry about what sort of shenanigans will be pulled prior to the midterms and various forms of disenfranchisement continue, abetted by the court system, but what happened in Hungary last month shows the solution. If people will just bother to vote at all, the balance of power will shift, no matter how heavy the thumb on the scale. We don’t have a voting problem in this country as much as we have a non-voting problem. When half the electorate sits home, an energized minority can grab outsize influence due to the winner take all nature of our electoral system.
The Supreme Court’s decision this week in Louisiana v Callais which basically invalidates the Voting Rights Act. Spits in the eyes of John Lewis, Thurgood Marshall, and Martin Luther King Jr. and then dances on their graves. I’m expecting a repudiation of Brown v Board of Education next. Gerrymanders can be undone. It requires time, patience, and energy. Movement conservatism has been playing a long game for more than fifty years to achieve the ascendancy they currently have. And it started with movement conservatives taking over the structure of the party at the grassroots level by doing the thankless work of precinct committee chairs and the other nuts and bolts requirements of local governance. They volunteered and stepped up at the municipal and county level. They never focused on losses or setbacks other than to learn from them for the next election. They found individuals willing to commit resources to building an infrastructure which would help reframe public debate on social issues. They identified allies and came up with causes around which they would rally.
Progressives need to remember that all politics are local and that change starts at the bottom and works its way up. You can’t start at the top. Moving public opinion requires time and careful incremental changes. Anything too rapid that takes the general population outside of their comfort zone, even when it’s the right thing to do, will always provoke a backlash. Our current backlash is, of course, moving from carefully coded to overt racism and in a lot of quarters is bringing outright white supremacy into the public conversation. I am hoping that this proves too rapid too quickly for the other side and that there will be a backlash which will push us away from some of the more odious policies of the current administration. The white wine moms of Minnesota went to bat for their Somali neighbors and things changed.
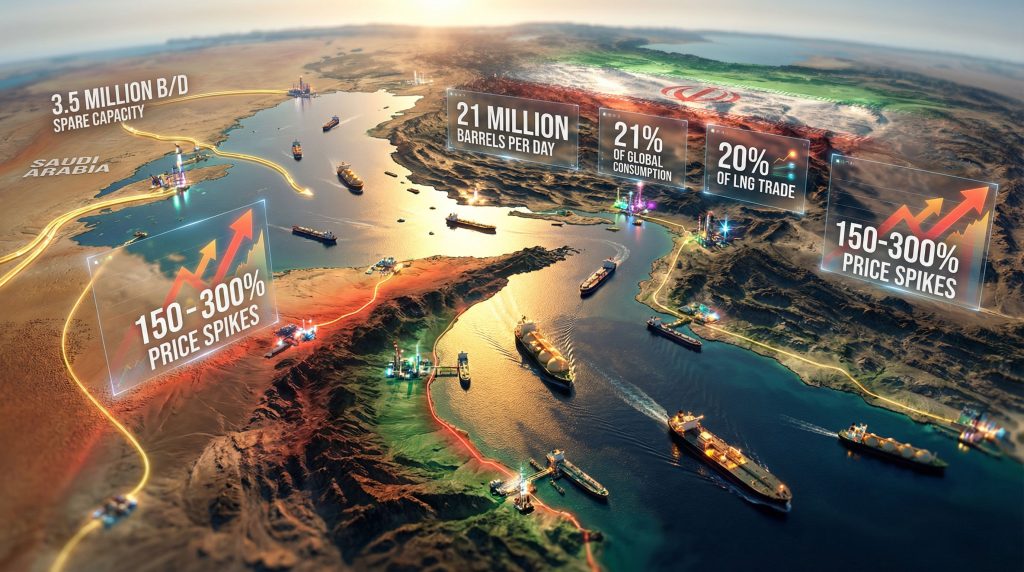
War in Iran (which may or may not be ongoing – the White House can’t seem to come up with a consistent policy on that one), an attempted assassination (which appears to be exactly what it seems – a lone figure tired of waiting for those with the power to do something about evil action deciding to take matters into his own hands), a ballroom cum bunker that no one asked for or wants have driven the immigration story off of the front pages but it’s still very much out there. Markwayne Mullin is smart enough not to treat the post of DHS secretary as some sort of self-aggrandizing continuous Vogue cover photoshoot but he’s busy continuing what Kristi Noem put into place and Stephen Miller is still giving the marching orders. We continue to build out concentration camps, have an untrammeled federal law enforcement arm in ICE reveling in inflicting misery, ship lawful residents overseas to countries where they have no resources and ties (including unaccompanied minors and in a couple of cases US citizens), and in general flout the rule of law. I say we because all of these people, in theory work for us – we, the people. We either voted for this or did not convince enough of our friends and neighbors to vote against this.

The weaponization of DOJ continues apace as Trump continues on his revenge tour. The indictment of James Comey over a photo depicting ‘8647’ spelled out in seashells on a beach is one of the more ludicrous uses of taxpayer dollars in recent memory. ’86’ has been around in American slang since the 1930s. It came out of the shorthand waitstaff and cooks used in diners and meant ]’to throw out’ or ‘not available’. It has never meant to kill or to assassinate. It’s not a threat, it’s protected free speech under the first amendment, and I haven’t seen DOJ try to indict anyone from the Trump campaign for selling merchandise labeled ‘8646’ during the 2024 election season – and there was plenty of it. I’m no fan of Comey. His insistence on reopening the FBI investigation into Hillary’s emails in 2016 may have done more than anything else to gift us with the Trump presidency so maybe this is karma. Then there’s the unwise indictment of SPLC for paying informants in white supremacy organizations for the inside scoop. Those at the top of DOJ aren’t the brightest (those have all departed a department focused on ideology and vindictiveness for more satisfying careers) but the lawyers at SPLC are still pretty savvy and have wasted no time in showing that the feds have known about their informant programs and shared in them for decades. I predict that case will quietly disappear.

I’m about to start throwing myself into The Tempest as I get my ideas and concepts ready for production this summer. If you’re interested in being part of it, let me know. First rehearsal is June 22nd, Tech starts August 1st and it runs the weekends of August 6th and 13th. I’m unpacking a lot of the subtext at the moment and trying to decide which themes to emphasize. There’s a lot about imperialism and oppression. There’s manipulation, betrayal, familial bonding, love, the power of the natural world. It’s a lot, like all Shakespeare. I think I’m going to lean into the more positive and mystical elements but want to acknowledge the others are there. Perhaps the ultimate theme is one of balance. Things are out of balance at the start with the storm and Prospero’s displacement but by the end the pieces fall back into place and balance is restored.
And perhaps that’s how we need to view what’s going on in the US right now. We are definitely out of balance. Those in ascendancy feel that they have the right to carry us back to Jim Crow (and are busy calling special state legislative sessions to do it) and that the hopes and dreams and futures of people not like them are really not their concern. But don’t we do better when we make policies that cater to all of us in all of our crazy polyglot diversity? If we look at the historical record, more open societies are those that have made advancements in the arts and sciences and standard of living. Societies that close themselves, especially in strictures of religious fundamentalism, fossilize. They may go on but change, not stasis, is the engine of progress.
It was the anniversary of Tommy’s death this past week. It’s hard to believe it’s been eight years. And it will be twenty-five since Steve’s been gone this coming August. I’m getting old.