
Birthday weekend is over. I’m now firmly ensconced in a new decade. I hope the pattern of my life where the odd decades are disasters and the even decades pretty wonderful prevails and that I have a great ten years coming up. Who knows though? Wouldn’t it be nice to have powers of divination and be able to identify and plan for the pitfalls in advance? Unfortunately. given my usual life patterns, I would end up as a Sibyl Trelawny with true clairvoyance only at inopportune moments and with perplexing results.
The big birthday bash came off on Saturday night with all of the hitches firmly backstage. The attendees all seemed to have had a good time. I viewed it as a chance for me to give something back to the community that has supported me through the last four years of hell between widowerhood and pandemic. It’s been a long time since I’ve hosted a snazzy catered affair and it will be a long time before I agree to do so again. Too many details to parse through and too many bills at the end of the evening. Maybe on my 70th should I make it that far…
A friend, who had been invited, committed suicide just a couple of days before the party. I first met him when he was a medical student at UAB, one of the few out gay male students at the time. There were very few out gay male faculty and as one of the few, I was the advisor to the fledgling LGBT student group of which he was president. Not only was he a brilliant student, in the MD/PhD program, he was also a musician. I sang with him in the opera chorus, our church choir, and Tommy wrote an oboe piece for him and our choir director to play for one of the children’s holiday pageants he put together. He graduated from med school, went off elsewhere for advanced training and returned to Birmingham to join the faculty in the Department of Pathology about a year ago. I saw him some after his return, but not a lot, the pandemic having disrupted so many patterns and activities.

I don’t know and cannot hope to know what made him think he had no other options. I’m not so much sad as mad at the tragic waste of a life and brain. And I expect more young health care professionals of my acquaintance are going to take the same route over the next few years. The healthcare industry is fundamentally broken and the pressures of that crack up are coming to rest on the shoulders of the more junior providers who have the least ability to change their lives as dictated by higher ups and the least experience and resilience to cope with those dictates.
I’ve expected the American healthcare system, excuse me American healthcare industry, to break within my lifetime. I was just wrong about when that would happen. I was expecting it to happen in the decade of the 2030s under the pressure of demands from the aging baby boom – a combination of enormous demographic numbers and unrealistic expectations as to what healthcare can and cannot do. Instead, it’s happening in the 2020s under the pressures of two years of pandemic combined with a general unraveling of American society through loss of trust by the citizenry in institutions and expertise. Those of us who have weathered the last two years, are emerging somewhat shell shocked, no matter the specialty or how tied in to the acute medical issues of the pandemic it may be. This is being compounded by a steady exodus of providers to the exits of retirement or career change, leaving fewer and fewer people to handle the workload, nudging up due to demographic and other factors.

Two years of disrupted patterns have also created some other trends. One, administrative types in the health care system, many of whom spent the majority of the pandemic at home, began to explore the capabilities of big data systems fed by electronic health records. I’m sure much of what they are learning is very useful but the gathering and entering of that data trickles down to providers who are already very pressed for time. Two, patients and families became much more adept at online access to providers through these new data systems and the number of lengthy notes, downloaded blood pressure graphs, photos of funny looking rashes, complaints about valet parking, and other communications have risen exponentially. In some systems, adept nursing staff can intercept and handle some of these before they ever reach my desk but other systems, in order to save salary costs in the ambulatory environment have replaced nurses with medical assistants who have neither the knowledge base or critical thinking skills to address most of this so it all ends up on the desks of me or my colleagues. The end result is the ambulatory workload is skyrocketing without a lot of hope of curbing the trends as there are fewer and fewer providers opting for ambulatory careers and the system, having to absorb the costs of the pandemic, is trying to control costs elsewhere in the system and is loathe to add support staff.
It takes a minimum of eleven years (and usually more – I had thirteen years) of higher education to create a well trained physician. Any solutions posed today won’t begin to make inroads for another decade or so. There’s been a significant move towards nurse practitioners and physician assistants to handle the shortfall (they can be produced in about half the time of a physician) but I am of the opinion that, especially in geriatrics, the greater depth of knowledge inherent in physician training is what patients deserve. Unfortunately, if we’re tasked with spending most of our time on data entry, we don’t really have the time to spend thinking about how to better handle our complex cases. I wish I had a solution to these dilemmas. I don’t. I can only lay them out in easily understood terms.
As the healthcare system starts to fail, more and more patients won’t be able to get what they need from it. There are very few ambulatory services (mine included) that has room for a new patient in less than four to six months – an inappropriate lag time for urgent or emergent issues. The last few reports I have from the emergency rooms are for multi-hour waits. There is a nationwide shortage of IV contrast for imaging studies so anything not emergent inpatient is being bumped back for months. Appointments for mental health services are practically nonexistent. And all of this is without a major Covid surge in the area. It’s going to get worse. Buckle up.
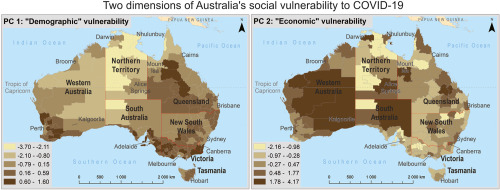
There was an interesting piece in the New York Times this weekend that suggested that if the US had responded to the pandemic in a way similar to Australia (a country very like ours culturally and economically), roughly 9/10 of the dead would still be alive. That’s 900,000 people that didn’t need to die. The major difference between us and Australia? Trust. Trust in science, trust in government institutions, trust in the health care system, trust in each other. The last decade or so, fed by the media and our political system, has been all about destroying trust in our institutions and in each other. The fault lines have been drawn. The partisans are in the stands, each cheering on their team, red on one side and blue on the other, as the players savage each other on the field. Nearly a million people have died that didn’t need to and we are so ill prepared as a society for the next crisis, which will also likely be politicized for monetary gain, that I can see this pattern happening over and over again. There’s no easy way to rebuild trust once it has been shattered. All I know how to do is try and live a valid life open to everyone and all ideas.