
I’m getting a lot of complaints from patients and their families about the lack of timely availability of specialty and other services these days. There isn’t a day in the office where I’m not having to try to end run scheduling software in order to get someone something before next March. It’s become yet another daily task for which I was left unprepared by medical school. We didn’t have classes in data entry either but that’s become a big piece of what clinicians have to do these days. Fortunately, my high school career as a keypunch operator gave me certain skills that I have retained. I suppose I have come full circle. The requests for additional data fields that have no clinical relevance in some parts of my job have required me to put my foot down occasionally. The data is there and the administrative office that wants it can hire an abstractor rather than make me fill out yet another form.
My patients keep asking me why the American health system, at least form their point of view, is falling apart. It’s a complicated question without an easy answer but I’ve been able to piece some things together and, of course, a good deal of it is pandemic related. I think we’re all going to continue to find that a lot of the changes that are coming in our society over the next decade will be traced back by historians to the pandemic and political upheavals of the last five years or so. Don’t expect any of this to end any time soon. The closest analog is likely the impact of World War I and the 1918-19 flu pandemic. Take a look at the society of Titanic (1912) and The Great Gatsby (1923) – only eleven years apart but everything has changed.
Once upon a very long time ago in the spring of 2019, I had an idea for a book. It was to be called Boom! and, as I leisurely wrote it over the next five years or so, it would come out in the mid 2020s explaining how the health care system would be changed by the pressures of the aging Baby Boom which would start needing geriatric care en masse starting in the late 2020s and early 2030s. I wrote a couple of chapters over that spring and summer and then, as fall arrived, got caught up in various theatrical endeavors so I put it aside to work on again in the spring of 2020 when the theater season would be slowing down for summer. Nature, of course, had other ideas and upended all of our lives in March of 2020 and I, as part of my coping with wrenching change, began these writings, completely unaware that they would morph into what is now two and almost certainly to become three volumes of The Accidental Plague Diaries. The rough chapters of Boom! were transformed into some of the material that has gone into these essays – perhaps I’ll pull it out again and rework it and Boom! will live again. Perhaps not. I’ll just have to put aside those daydreams of being hailed as a clairvoyant as my predictions regarding the health system came true.
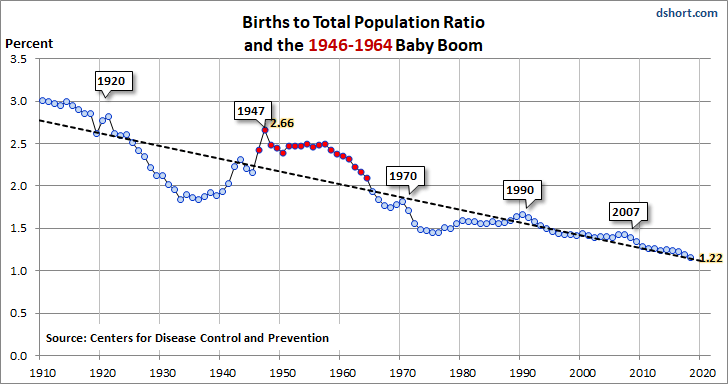
The pandemic put various trends that were already present on steroids and so here we are in 2022 starting to have problems that I thought we wouldn’t see for another five to ten years. The inability to provide services in a timely fashion is a key one. I won’t say that the US health care system is irreparably broken at this point, but it’s definitely on the critical list and it’s going to take some major changes in policy to right the ship. If that doesn’t happen, we’re going to see continued and worsening delays in the system and people will die as they won’t be able to get what they need when they need it.
So why is this? The first pandemic related reason is departure of skilled clinical staff. This doesn’t just apply to providers but to all of the other professions that make up modern health care – nurses, therapists, social workers, pharmacists, dietitians… the list goes on. Being on the front lines in the early pandemic prior to the availability of vaccines meant that some died or developed long covid related health issues that kept them from working. The older generation used the pandemic as a reason to retire. Loss of other family members forced some to leave the work force to take over as caregivers for suddenly parentless children or family elders who no longer had a consistent adult to help them at home. Most of these positions require a highly skilled individual with many years of training and licensure requirements. They can’t be created from scratch in a year or two. Personally, I had thirteen years of higher education. When everyone has a job, there’s no one left to hire. (Our current anti-immigration sentiment, even against highly skilled immigrants isn’t helping).
Tangential to this is that a lot of the departures to retirement are of senior individuals with decades of experience who are adept at caring for large panels of patients. It’s not something you can do right out of training. You have to have a great deal of real world experience to learn how to juggle all of the balls at once. I didn’t really become good at my job until between five and ten years after completing my training. That was now twenty years ago so I feel like I’m really good at it at this point but there are very few around who could step up and do just what I do. Every one that retires throws hundreds to thousands of patients back into the system looking for new medical care and snatching up new patient appointments.
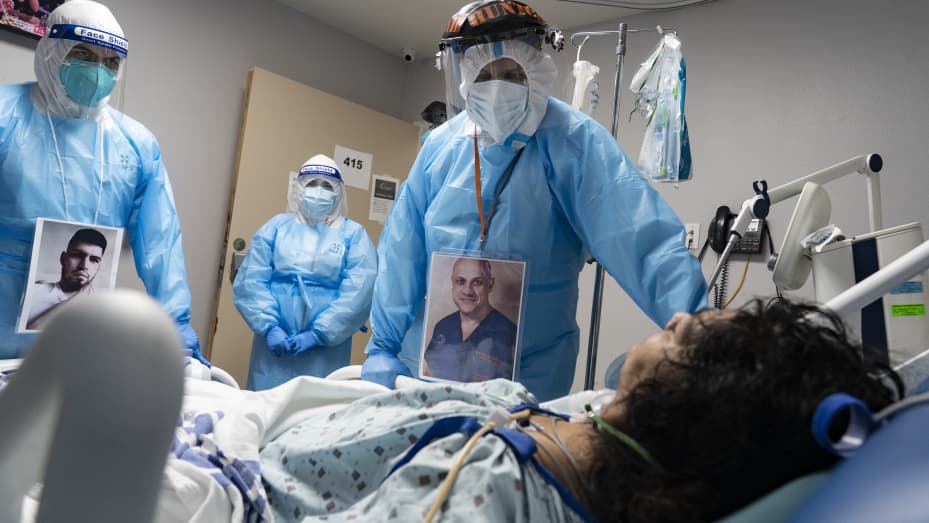
The pandemic also prevented the system from operating normally for several years. It’s only really gotten back to working in its usual way this past summer. Two years of seat of the pants ad hoc medicine and postponement of routine procedures and screening tests means two years of disease that might have been detected early getting away and presenting at a more advanced and complicated state requiring more intensive treatment and more appointments. There’s a huge backlog of mammograms and colonoscopies and other such things that have to be worked through. I would like to think that we’ll be able to operate normally going forward but I’m not so sanguine in thinking that everything is over. New variants keep circulating and human nature, politics, and inertia are keeping people of getting their boosters.
After the pandemic, the next most important issue is demographics. Here comes the Baby Boom. The lead edge will turn 77 next year and the years form 75-85 are generally when individuals start to transition from the robust health of late middle age to the collections of chronic diseases and dysfunctions that characterize old age. The Greatest Generation and the Silent Generation (to which most of my current patients belong) tend to be a stoic and accepting lot who understand that as their bodies age, things will change and they aren’t happy about it, but they do get the basic biological issues that aging presents. The Baby Boom is not of this mindset. They consider themselves forever young and the problems of aging, being diseases, must therefore have cures and they must have them dealt with and removed now, thank you very much, for they are interfering with their life plans. As they continue to age, more and more of their problems will not be amenable to any sort of curative treatment and they are not going to like that one bit and make demands of the health care system that cannot be met. There is also the impact of their huge numbers. The Baby Boom in the US has had 10,000 people a day celebrating their 65th birthday since the first ones did on January 1, 2011 and that won’t end until December 31, 2029. We haven’t substantially increased training programs for health care providers since the turn of the century despite this demographic imperative. It’s too expensive.
Politics comes into play. The passage of the Patient Protection and Affordable Care Act (Obamacare if you will) substantially altered the US health insurance market and, in the decade or so since its implementation, the number of uninsured has fallen from about 15% to about 5% nationwide. This is a laudatory goal (and has anyone else noted that the Republican Party is no longer introducing bills to repeal Obamacare ever other week?) but it has had the effect of granting an additional thirty million people or so easier access to the system and all of them are wanting and should be entitled to services.
Then there are the rather peculiar capitalistic beliefs under riding American medicine. In most countries, the health system is studied and planned and the pieces are designed to maximize the health of the population and to provide the widest possible service for the lowest possible cost. This means the types of specialties are controlled to the needs of the population, not the needs of the stockholders of hospital corporations or other such motivators. Our system is more of a free for all. There are limitations on the number of specialty training positions but less popular specialties, which tend to include those that provide the majority of ambulatory care are often going begging. We need about 35,000 geriatricians in the 2030s and 2040s due to the needs of the Boom which will be in their 80s and 90s during that period. We have about 6,000 currently and we’re only producing about 200 new ones a year, just enough to offset retirements.
Put all of these things together and, yes, you’re going to have to wait for that appointment. I’ll do my best for you. I’ll pull strings when I can. But it’s just where we are.